How to Treat Heel Spurs
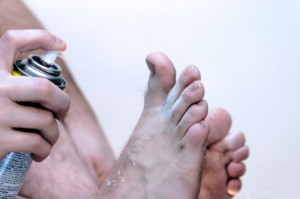
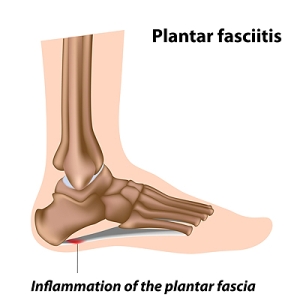
Heel spurs are calcium deposits that cause bone protrusions on the heel bone. Heel spurs are usually associated with plantar fasciitis, which occurs when the plantar fasciitis in the foot becomes inflamed. Typically, heel spurs don’t cause any symptoms. However, they can produce chronic or intermittent heel pain. Those who have had the condition often describe the irritation as a stabbing pain.
There are risk factors that may make you more likely to develop heel spurs. People who have abnormal walking gaits, run and jog on hard surfaces, are obese, or wear poorly fitting shoes are more likely to develop heel spurs.
Fortunately, there are precautions you can take to avoid developing heel spurs. One of the best ways to do this is by wearing well-fitting shoes with shock-absorbent soles. Another preventative technique is to choose running shoes if you plan on running, and walking shoes if you plan on walking. Shoes are made for different activities and it is important to research a shoe before you purchase a pair.
The pain associated with heel spurs often decreases the more you walk. However, a recurrence of pain after an extended period of rest or walking is likely to occur with this condition. Those with severe heel spur pain may opt to go the surgical route for treatment. However, more than 90% of those with the condition get better without surgical treatment. If you have a heel spur and want to know if surgery is right for you, you should go to your podiatrist and he or she will be able to conduct a pre-surgical test or exam to determine if you are an optimal candidate for surgery.
The Risks of Peripheral Artery Disease
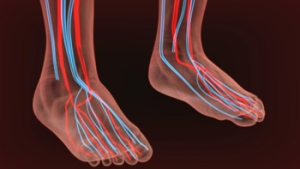
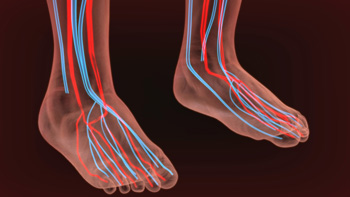 Peripheral artery disease (PAD) is a medical condition in which the blood vessels in your lower limbs narrow or become clogged due to the buildup of arterial plaque. This reduction in blood flow means that you have poor circulation, which increases your risk of developing a whole host of potentially serious medical complications, including strokes, heart attacks, and aneurysms. Left undiagnosed and untreated, PAD in your lower limbs can advance to the point where there is limited to no blood flow, resulting in the death of the muscles in your lower limbs and increasing your risk of needing a limb amputation. Fortunately, PAD is easy to screen for and can usually be managed with lifestyle changes and medication, especially if it is detected in its earliest stages. Symptoms of PAD in the lower limbs include pain or cramping while walking, swelling, numbness, skin discoloration, and poorly healing sores. If you experience any of these symptoms, it is strongly recommended that you consult with a podiatrist who can screen for PAD and provide you with treatment options.
Peripheral artery disease (PAD) is a medical condition in which the blood vessels in your lower limbs narrow or become clogged due to the buildup of arterial plaque. This reduction in blood flow means that you have poor circulation, which increases your risk of developing a whole host of potentially serious medical complications, including strokes, heart attacks, and aneurysms. Left undiagnosed and untreated, PAD in your lower limbs can advance to the point where there is limited to no blood flow, resulting in the death of the muscles in your lower limbs and increasing your risk of needing a limb amputation. Fortunately, PAD is easy to screen for and can usually be managed with lifestyle changes and medication, especially if it is detected in its earliest stages. Symptoms of PAD in the lower limbs include pain or cramping while walking, swelling, numbness, skin discoloration, and poorly healing sores. If you experience any of these symptoms, it is strongly recommended that you consult with a podiatrist who can screen for PAD and provide you with treatment options.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Michael A. Wood from Foot Health Institute. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
How to Find Shoes That Fit Right
 Did you know that your shoe size can change even in adulthood? Many people may actually be wearing shoes that are too big or too small because they are unaware of changes in the size of their feet. Wearing the wrong size shoe can lead to a variety of foot problems, from heel pain to hammertoes and everything in between. For this reason, it is important to have a proper shoe fitting. This can be achieved at a brick-and-mortar shoe store, where salespeople can assist you in finding the right size, and where you can try on the shoes for yourself before you buy them. Going shoe shopping later in the day, when your feet are at their largest, can help ensure that you purchase shoes that will fit your foot properly throughout the whole day. A podiatrist can also help you find the right shoes, can prescribe custom orthotics to correct certain foot problems, and can offer treatment for various foot conditions as needed.
Did you know that your shoe size can change even in adulthood? Many people may actually be wearing shoes that are too big or too small because they are unaware of changes in the size of their feet. Wearing the wrong size shoe can lead to a variety of foot problems, from heel pain to hammertoes and everything in between. For this reason, it is important to have a proper shoe fitting. This can be achieved at a brick-and-mortar shoe store, where salespeople can assist you in finding the right size, and where you can try on the shoes for yourself before you buy them. Going shoe shopping later in the day, when your feet are at their largest, can help ensure that you purchase shoes that will fit your foot properly throughout the whole day. A podiatrist can also help you find the right shoes, can prescribe custom orthotics to correct certain foot problems, and can offer treatment for various foot conditions as needed.
Finding a properly-fitting shoe is important in reducing injuries and preventing foot problems. For more information about treatment, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor will treat your foot and ankle needs.
Proper Shoe Fitting
A common concern when it comes to foot health, having properly fitted shoes can help prevent injuries to the foot. Out feet affect our posture and gait, which in turn affects the biomechanics and overall bodily structure. With 33 joints, 26 bones, and over 100 ligaments, the potential for serious injury is much greater than one realizes. Although the feet cease growth in adulthood, they still change shape as they mature. Here are some factors to consider when it comes to investing in proper fitting shoes:
- Be sure the shoes fit correctly right away
- Ensure the ball of your foot fits comfortably in the widest portion of the shoes
- Even though they may look fashionable, improper fitting shoes can either create adverse conditions or exacerbate existing ones you may already have
- Walk along a carpeted surface to ensure the shoes comfortably fit during normal activity
Keeping in mind how shoes fit the biomechanics of your body, properly-fitting shoes are vitally important. Fortunately, it is not difficult to acquire footwear that fits correctly. Be sure to wear shoes that support the overall structure of your body. Do your feet a favor and invest in several pairs of well-fitted shoes today.
If you have any questions please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Proper Shoe Fitting
When it comes to maintaining foot health, wearing properly-fitting shoes is important. While wearing the appropriate pair of shoes may seem like a trivial concern, the reality is that improperly fitted shoes cause an astounding amount of injuries to the feet. The overall structure and the biomechanics of our bodies are directly affected by our posture, gait, and feet. Because of this, pain and discomfort felt throughout the body are often related to a problem in the feet. And, most foot problems usually stem from improper footwear.
Shoes should not be purchased with the expectation that they will easily stretch and contort to the size and shape of your feet. When shopping for footwear, look for shoes that fit correctly and comfortably as soon as you put them on. Do not purchase shoes that are too large or that slip in the heel area when you walk. Do not choose shoes that are loose with the intention of wearing thicker socks to compensate for the space. The widest portion of the shoe, the ball of the foot, must be made sure to fit comfortably in the shoe.
Keeping all of these suggestions in mind may be difficult when shopping and when trying to select from a wide array of different shoes. Nonetheless, your time and money will be wasted if you purchase a pair of shoes that are too uncomfortable for you to actually wear them. After finally selecting and purchasing a pair of shoes, try them on at home. To truly ensure whether or not your shoes fit comfortably with normal activity, walk around on a carpeted surface to determine how they feel on your feet.
The possibility of damaging your feet’s 33 joints, 26 bones, and 100+ ligaments is much higher than many people suspect. Finding an appropriate and properly-fitted pair of shoes is perhaps the single most important action you can take to maintain excellent foot health and help prevent injury. The fact that our feet continue to change with age is one that many people often forget. Even if our feet no longer change in size when we mature, our feet will still change in shape.
If you already have pre-existing foot problems, there is a greater possibility that wearing improperly-fitted shoes will worsen those problems. The good news, however, is that appropriate footwear is not difficult to find. While shopping for shoes, remember that improper footwear can detrimentally affect the feet, the entire body and its biomechanical structure as well. The shoes you wear can greatly impact your legs, back, and entire body, as your posture and gait are related to your feet. Finding and selecting the best properly-fitted shoes is necessary in achieving optimal health.
How to Prevent Athlete’s Foot
Athlete’s Foot is a common fungal infection of the foot. The fungus that causes athlete’s foot, known as the tinea fungus, thrives in dark, warm, moist environments. This makes areas that are often tightly covered and sweaty, like your feet, a perfect breeding ground for tinea fungus. To prevent athlete’s foot, it’s important to keep your feet as dry as you can. Avoiding wearing tightly-fitted shoes, which can trap moisture, and frequently changing your socks can also help in the prevention of athlete’s foot. If possible, wear open-toed sandals, which will allow more air to circulate to your feet and decrease sweating. Open-toed sandals also have the added benefit of exposing your feet to sunlight, which helps slow the growth of the fungus. If you suspect that you may have athlete’s foot, consult with a podiatrist who can diagnose and treat the problem.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. Michael A. Wood from Foot Health Institute. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Heel Pain and Plantar Fasciitis
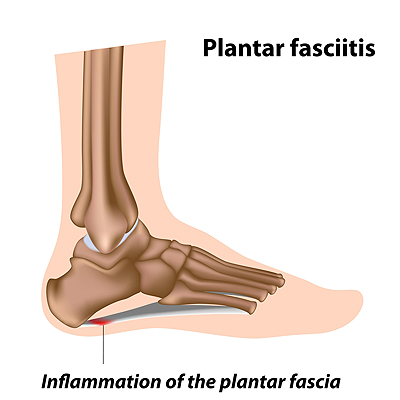 The plantar fascia is located on the sole of the foot, and its function is to connect the heel to the toes. The chronic foot condition that is known as plantar fasciitis can develop from wearing shoes that do not fit correctly, or from standing on hard surfaces for the majority of the day. This may cause the plantar fascia to become inflamed. A common symptom that patients often notice is severe heel pain that may be more pronounced in the morning after arising. An effective prevention technique can be stretching the calf muscles. This can be practiced by standing on a step, and gently lowering one heel at a time. Additionally, it may help to roll the affected foot on a tennis ball, and this may help to stretch the heel. If you are experiencing heel pain, it may be indicative of plantar fasciitis, and it is advised that you seek the counsel of a podiatrist.
The plantar fascia is located on the sole of the foot, and its function is to connect the heel to the toes. The chronic foot condition that is known as plantar fasciitis can develop from wearing shoes that do not fit correctly, or from standing on hard surfaces for the majority of the day. This may cause the plantar fascia to become inflamed. A common symptom that patients often notice is severe heel pain that may be more pronounced in the morning after arising. An effective prevention technique can be stretching the calf muscles. This can be practiced by standing on a step, and gently lowering one heel at a time. Additionally, it may help to roll the affected foot on a tennis ball, and this may help to stretch the heel. If you are experiencing heel pain, it may be indicative of plantar fasciitis, and it is advised that you seek the counsel of a podiatrist.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Michael A. Wood from Foot Health Institute. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Lansing, and Chicago, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.